In 2017, assisted dying, that is the ability to request that a physician provide help in ending the life of a person with an incurable disease became legal. Much like changes to same-sex marriage and prostitution, this was a major policy change that was significantly driven by the courts (Carter v. Canada). Public opinion moved in a permissive direction over the past decades. Public support in the polls arguably made policy change difficult. Canadians ultimately got part of what they wanted with the legislation.
Was this helpful for policy makers? Could public support be easily responded to within an environment in which critical questions about the implementation of assisted dying would strike at the very core of key health and religious institutions? It was a challenging task.
In the end, the legislation introduced and passed by Parliament struck a balance between the right to assisted dying and other considerations. Most notably, the Act required the person to be 18 years of age and to have a grievous and irremediable medical condition. In addition, one needs to be mentally competent at the time of the assisted dying procedure. Overall, the balance struck by the legislation was generally aligned but not completely consistent with public opinion at the time.
Parliament ultimately looked at the assisted dying debate and did the minimal legalization possible.
The historical trend in Canada of support for assisted dying
Before considering the trend, it is worth considering the language challenge. Discussions about end-of-life options are inevitably caught up in the language we use to discuss and measure them. This is this an issue of question wording. It is also about the broader narrative that the terms are embedded. In the 1950s and 60s, Gallup focused on euthanasia and suicide. In Canada, the assisted suicide has given way to assisted dying as the term of most use.
The key language issues boil down to three things. First, who made the end-of-life decision? Second, who, if anyone, assists with the process of dying. Third, on what basis has the person decided to end their life (e.g. pain, terminal illness, etc.). Assisted dying has emerged as the main concept in Canada and has largely replaced euthanasia or assisted suicide. Unfortunately, most of our historical data uses these concepts.
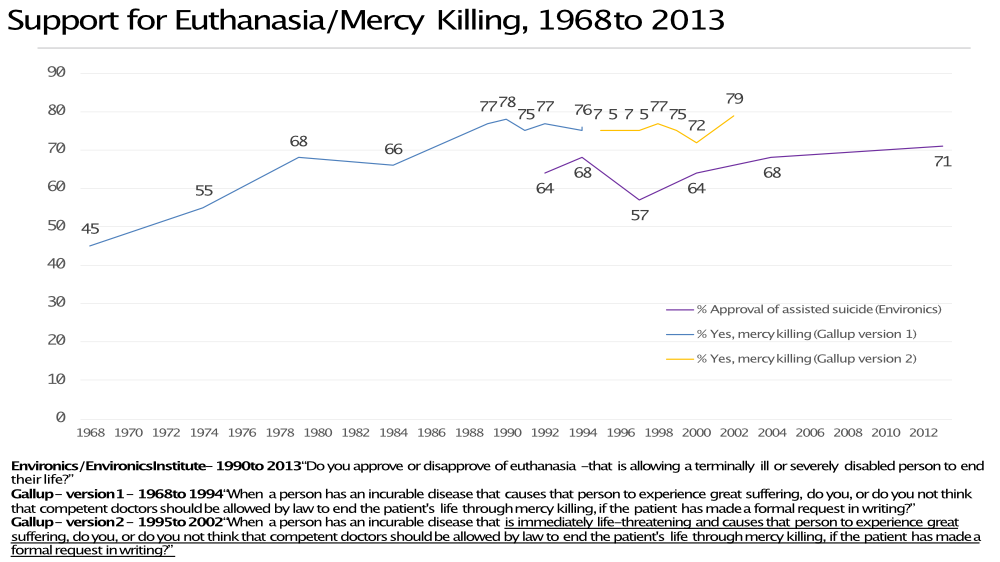
1968 to 2013: Gallup and Environics
In Canada support for assisted dying rose dramatically according to Gallup from the late 60s when less than half of the population supported the idea of mercy killing when a person has incurable disease that causes great suffering. By the early 80s the yes group was in the majority. Support continued to rise until reaching a plateau in the 1990s. Gallup changed the question to add a sense of immediacy — “is immediately life threatening” — but the overall level of support stayed fairly constant across six survey waves and in line with the earlier trend.
There is support for the view that question wording has an impact, though this is mostly a question of degree. The Gallup question shows significantly more support than the Environics question. That said, the two lines appear to run in parallel, except for the dramatic fall in support registered in 1997 by Environics. From these early trends, it looks like not much happened to public opinion since the 1990s. The main growth in support took place in the 60s, 70s and 80s.
There is no clear evidence of an effect of specific events. There were, however, several cases that were significant. The first, the Sue Rodriquez case brought the issue to rare attention. Although her fight did not change the law, it was clear by the early 1990s that opinion was more supportive of assisted dying than in the past. The other cases, including the Latimer case, were instrumental in keeping the issue on the public agenda.
No surprise that a significant amount of polling took place starting in the early 1990s.
Timeline: Key Events
- 1992-1994: Sue Rodriguez seeks physician assisted suicide but Supreme Court does not allow her appeal. She dies of assisted suicide.
- 1994-1998: Robert Latimer is convicted of second-degree murder in the death of his daughter.
- 2012 (June to October) Gloria Taylor, an ALS sufferer, successfully argues that the law discriminates against the disabled. BC Appeals Court in split decision overturns it.
- 2014: Quebec passes a law to allow terminally ill patients to have medical assisted dying.
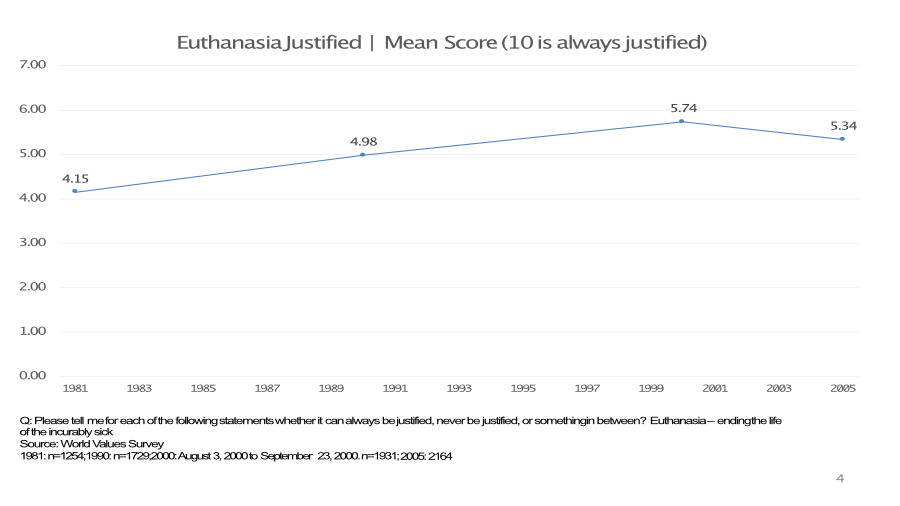
World Values Survey, 1981 to 2005
The World Values Survey also has tracked the views of Canadians. In this case, about whether “Euthanasia – ending the life of the incurably sick” is justified or not. Using a 10 point scale where 1 is not justified and 10 is justified, the figure below shows the mean. A higher value means a higher justification/ acceptance of euthanasia. Note in this case, there is no information about the agency of the person who dies. On this measure, acceptance of euthanasia increases in the 80s and 90s but drops somewhat in 2005. This is in contrast to the other tracking which shows rising or at least a stable trend. Unfortunately Canada has not been part of the WVS since 2005.
Pollsters have largely used the issue of assisted dying as a question of values. It is hard to see these trend questions as really informing public policy. The questions are too simple and often do not tackle all of the serious elements of what an assisted dying policy would look like. But as the Supreme Court decision neared, there are more and more questions that tap the issue.
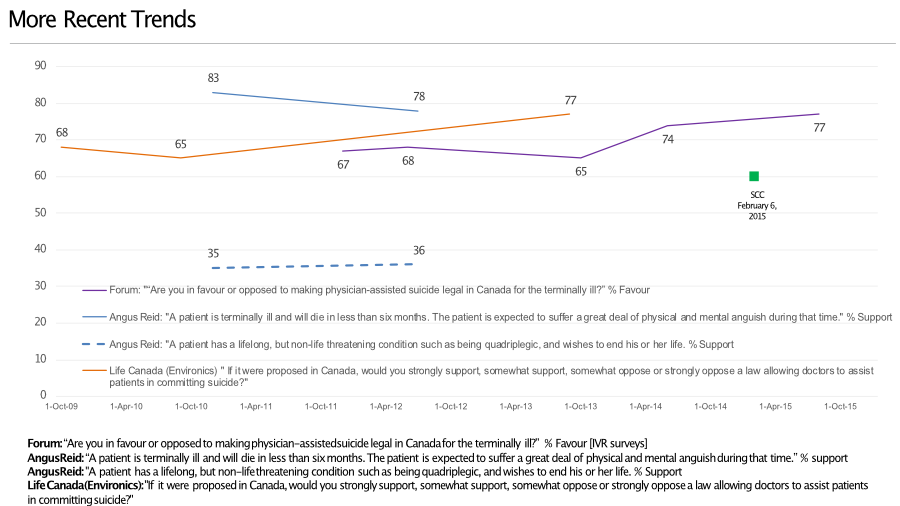
More recent trends
The number across the various questions are similar to the results from the longer time tracking. Life Canada, who have an interest in a particular position, tracking showed an increase in support for allowing doctors to assist patients to commit suicide. During the tracking the question intros changed slightly.
Forum data, which overlaps with Life Canada showed that the number of people in favour of making physician assisted dying legal increased. The Forum data is interesting because the Supreme Court decision falls within the tracking period. If attention to the case did anything, it raised or solidified public support.
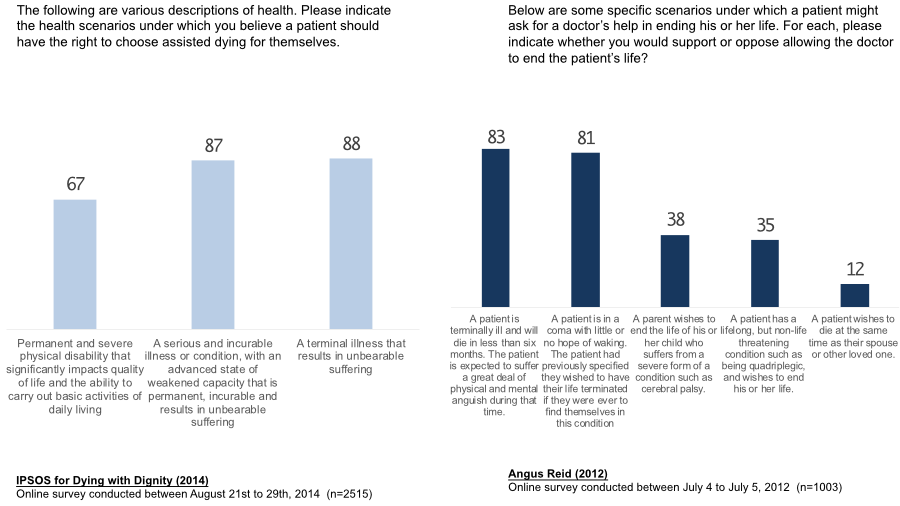
Finally, anticipating discussion about the constraints on approval for assisted dying, there is the Angus Reid data. Here, about eight in ten support allowing a doctor to help someone end their life if they were terminally ill, had less than 6 months to live and were expected to suffer a great deal. Note that only one in three or so would support it if the scenario involved someone with lifelong, non-life threatening condition.
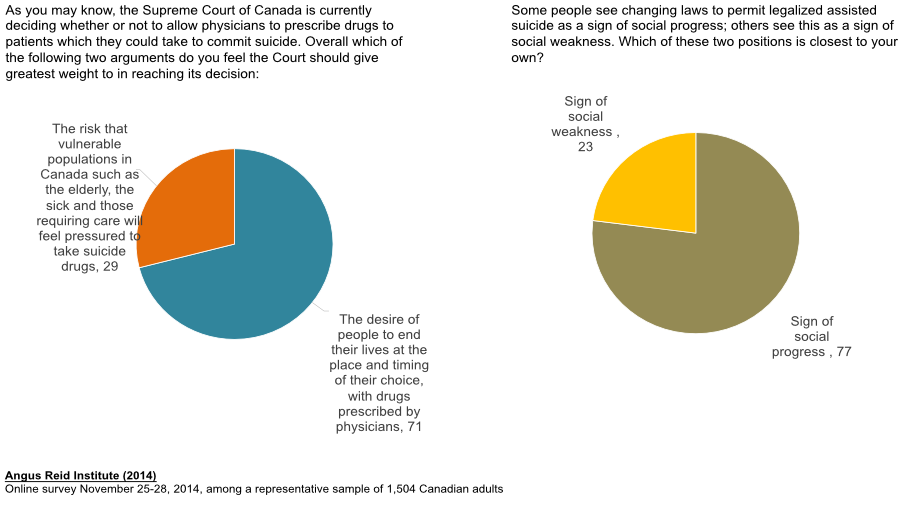
Public opinion on specific alternatives
If the public is definitely onside with assisted dying, as it appears to be, what should the policy look like. The overall similarity across questions, firms, and research methods suggests that most of the questions are tapping a value. That is, a general orientation. Or, it might not even be that. It could be a feeling. Or it might even be a judgment about what people like me should think.
Support is rooted in values. Before the Supreme Court ruled, a majority felt that the desire for someone to end their life should take precedence over the risk to vulnerable populations. Allowing assisted suicide was also viewed as a sign of social progress (77%) rather than a sign of social weakness. The Angus Reid survey shows that about 7 in 10 think of legalization in terms of individual freedom and control.
The eligibility requirements
We noted earlier that assisted dying for a non-life threatening condition is not as supported by Canadians. So how does the public think of assisted dying? The evidence is mixed but leans to a fairly permissive view of eligibility.
In the figure on the right, it is clear that Canadians in 2012 are not very supportive of extending eligibility to cases where things are not life-threatening. On the left, an IPSOS survey for Dying with Dignity shows that the highest support is for terminal illness with suffering (88%) or serious and incurable condition associated with suffering (87%). Only a minority do not support assisted dying.
Note that there is high but not as universal support for one scenario. If the disability is permanent and severe and significantly impacts quality of life, 67% would support assisted dying. There is no mention of suffering or the condition being terminal or in an advanced state. A majority supports assisted dying in this situation but it is not universal.
Attitudes about Eligibility
In 2016 the Angus Reid Institute tested a large number of eligibility considerations. Terminal disease and a great deal of pain are the two factors associated with support for assisted dying. Some considerations are almost universally associated with prohibiting assisted dying. For example, when a person’s care is perceived as a burden on their family. Viewed from this lens, assisted dying is a compassionate option and clearly the public would expect the scope to be quite narrow.
| Definitely Allow | Generally allow | Generally prohibit | Definitely prohibit | Total allow | |
| When a person has a terminal disease with a prognosis of, say, six months maximum and would rather end it sooner | 42% | 34% | 14% | 10% | 76% |
| When a person is in a great deal of pain | 36% | 37% | 17% | 10% | 73% |
| When a person can’t get access to medical care to treat their pain and suffering | 21% | 34% | 27% | 19% | 55% |
| When a person wants to control the exact time of their death to make things easier for their family | 16% | 29% | 27% | 29% | 45% |
| When an inmate serving a life sentence in jail wishes to end his/her life | 22% | 17% | 19% | 42% | 39% |
| When a person with multiple conditions like arthritis & diabetes feels overwhelmed and wants to die | 11% | 25% | 34% | 29% | 36% |
| When a person’s care is perceived as a burden to their family | 6% | 20% | 32% | 43% | 26% |
| When a person wants to stop spending their money in order to leave their family with a larger inheritance | 6% | 16% | 28% | 50% | 22% |
| When the cost of a patient’s care is very expensive to the health care system | 6% | 15% | 27% | 52% | 21% |
Assisted dying for mature minors
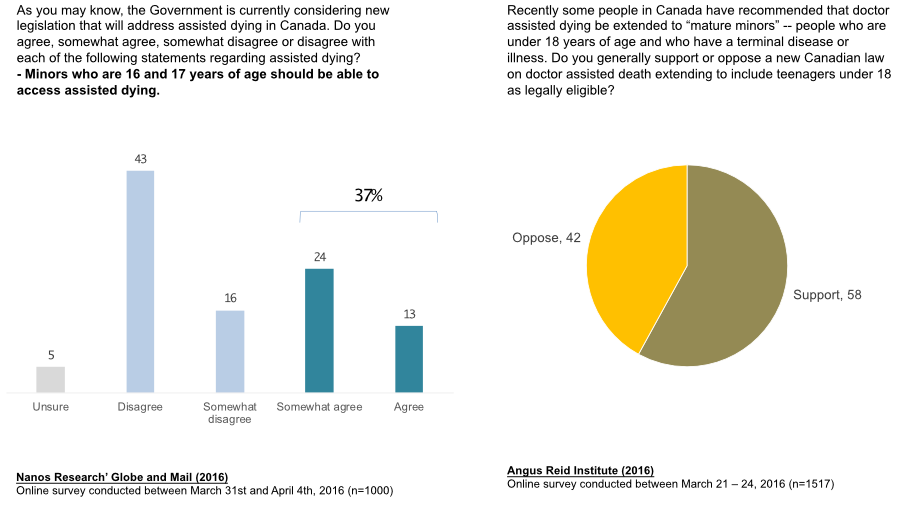
Assisted dying for minors is contentious. Public opinion is not clear on this question. A Nanos Research/ Globe and Mail found the publicly disagree with allowing minors who are 16 and 17 to access assisted dying. The 37% who agree represent about half the number of people who support legalization overall. An Angus Reid Institute (ARI) poll paints a somewhat different picture. Here, when told that the mature minor has a terminal disease, 58% support extending the eligibility.
We can only speculate about how to reconcile these two questions. Talking about minors without the context of a terminal disease appears to raise concerns, perhaps, that minors might do something they would regret. When reminded of the terminal disease, however, the overall drivers of support for assisted dying lead to a more supportive view. In the same ARI survey, when asked about support for mature minors in the case of psychological suffering, only 22% are supportive.
Observations
When it came to implementing the Supreme Court decision, the government of the day and ultimately Parliament took modest steps toward implementing assisted dying. Arguably they put in a regime that was as least permissive as possible. In so doing, they clearly choose a safe approach. Seven in ten Canadians are broadly supportive of legalization regardless of how it was framed in general. But the public viewed assisted dying through a very narrow lens — one shaped by compassion for those in pain and suffering.
The final legislation did not allow for advanced consent, excluded minors, and restricted the application of assisted dying to have a grievous and irremediable medical condition. The grievous and irremediable harm seems to be stricter than the public feeling. Many would also support extending assisted dying to minors in the case of terminal illnesses. There is also public support for advanced consent.
Canadians got legislation they mostly but not all of that they wanted. It addressed their humanist and individual freedom views of the world without taking too much risk. Of course, it took only a few years for the Superior Court of Quebec to strike down the “reasonable foreseeability of natural death” eligibility factor. Propose new legislation will make the law less restrictive. Part of this would allow a person whose death is foreseeable to waive the final consent required if there is a risk they will be incapacitated when the administration of the assisted dying it to take place. These moves are consistent with public preferences.
Canadian Institute of Public Opinion (CIPO). 2000. Gallup Poll, January 2000 [Canada]. [public-use microdata file]. Toronto, Ontario. Gallup Canada Inc. [distributor].
Environics Focus Canada [computer file]. Environics Research Group, Toronto, ON [producer], Canadian Opinion Research Archive, Queen’s University, Kingston, ON
Inglehart, R., C. Haerpfer, A. Moreno, C. Welzel, K. Kizilova, J. Diez-Medrano, M. Lagos, P. Norris, E. Ponarin & B. Puranen et al. (eds.). 2014. World Values Survey: Round Five – Country-Pooled Datafile Version: www.worldvaluessurvey.org/WVSDocumentationWV5.jsp. Madrid: JD Systems Institute.


